Click here for audio recording of this blog.
Summary
- The aerobic energy system is “broken” in ME/CFS and cannot be fixed with exercise (i.e., graded exercise therapy, also known as GET).
- The anaerobic (glycolytic) system appears to be somewhat functional in ME/CFS (but see McGregor’s work) and, in theory, can be trained to be more efficient with a carefully-designed exercise protocol done under the guidance of an ME/CFS-literate physical therapist.
- It is vitally important to avoid spending time above the anaerobic threshold, also known as “AT”.
- It is also advisable to minimize the duration of aerobic activities, including cognitive tasks.
- If the points above appear to contradict each other, in a sense they do! But a well-designed pacing program can minimize the negative effects of both aerobic and anaerobic metabolism while at the same time harness the benefits of each energy system.
Humility
This blog post was inspired by a conversation I had last week with a very kind and smart friend. She expressed curiosity about an idea but I wasn’t listening carefully and made some comments without taking the time to fully understand her question. She was very gracious and this gave me a chance to refine my thinking. It was also a reminder to be a better listener.
Our conversation centered on a 2016 talk by Mark VanNess from the University of the Pacific and Workwell Foundation. In the talk, VanNess presented a figure from a 2010 paper discussing what many with ME/CFS already know and experience: we have a broken aerobic energy system. For this reason, graded exercise therapy (GET) is a horrible idea. Proponents of GET assert that aerobic capacity can be improved by incrementally increasing exercise over time. While this may be true for people with other conditions, it has been disastrous for those with ME/CFS.
Instead, my friend was interested in the implications of the first two minutes or so of physical activity when we are briefly in anaerobic metabolism. I responded with knee-jerk comments about not exceeding the anaerobic threshold or “AT”, a central tenant of pacing, but my friend was asking about an entirely different issue.
A brief overview of energy systems
Before diving into the nuance of the discussion I had with my friend, a quick review of energy systems as they relate to ME/CFS might be helpful.
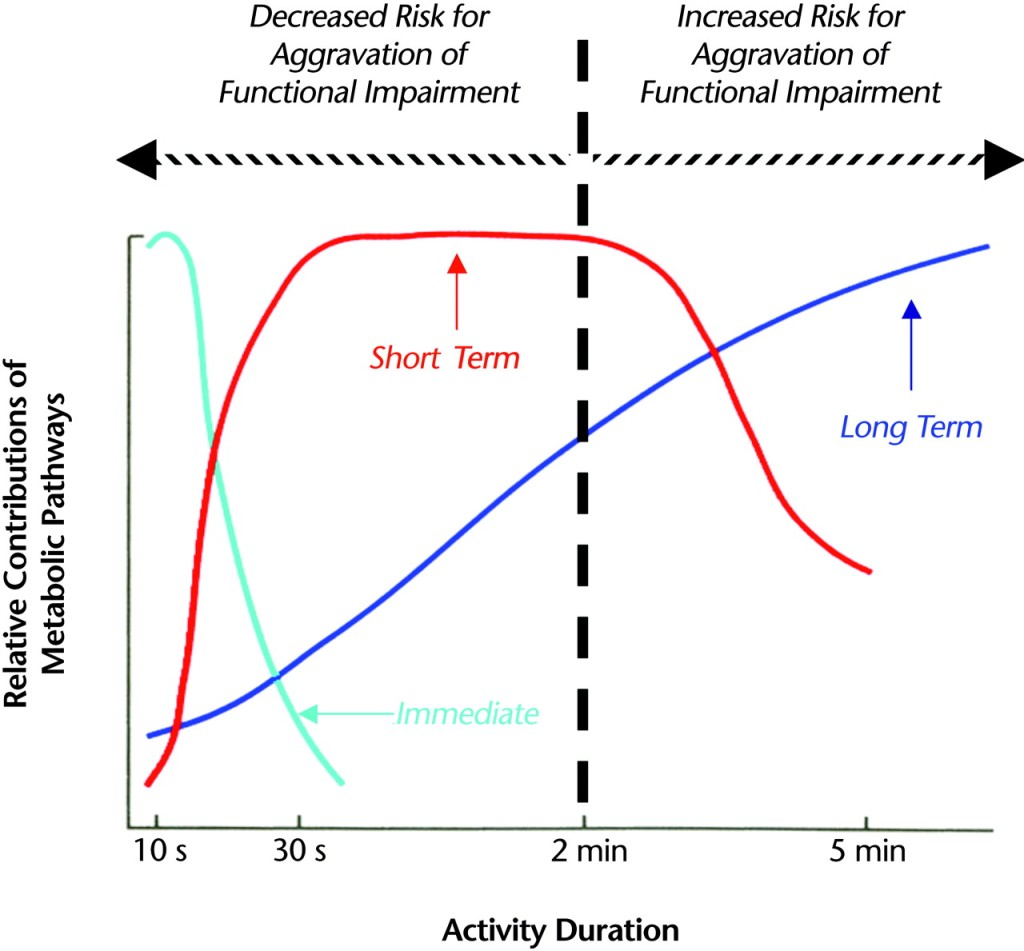
There are three main energy systems: the creatine phosphate (or phosphagen) system, the glycolytic system, and the oxidative system. After ATP is used up in the muscle, for the first 30 or so seconds of activity the majority of energy (ATP) produced is from the fast-acting but limited creatine phosphate system (labeled as “immediate” in Figure 1). For the next minute or so, most of the energy comes from anaerobic glycolysis (labeled as “short term”), but the aerobic system (labeled as “long term”) is also active to a lesser extent. Eventually, oxygen supply catches up with metabolic demand and increasingly more energy comes from the aerobic system.
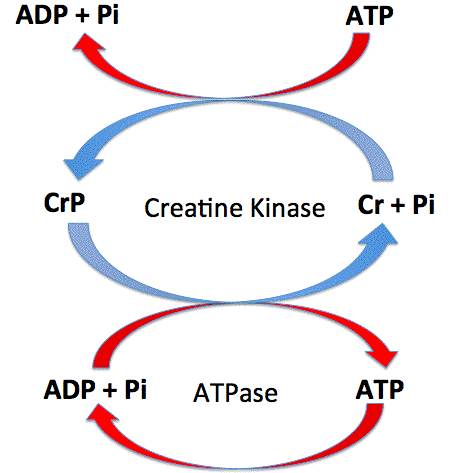
Creatine phosphate (CP) system: Creatine phosphate is stored in the muscles. Phosphate bonds release a large amount of stored chemical energy when broken. This energy is used to recycle ATP from ADP. However, muscles store a limited amount of ATP and CP and this is exhausted within a few seconds. This system provides rapid energy for contracting muscles and does not require oxygen.
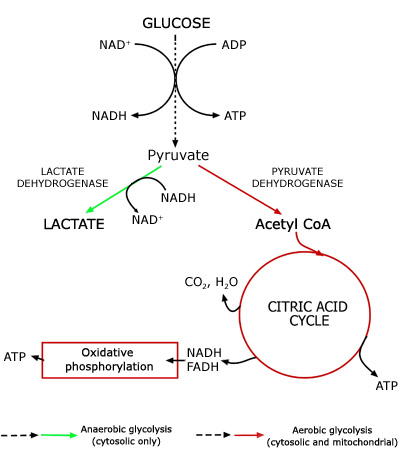
Anaerobic (glycolytic) system: Glycolysis refers to a series of 10 reactions that break down glucose into energy. Despite its apparent simplicity, there are many different intermediates and directions that glycolysis can take. When oxygen is limited lactate dehydrogenase (LDH) converts pyruvate, the end product of glycolysis, to lactate and when oxygen is present the pyruvate dehydrogenase enzyme complex (PDH) converts pyruvate to acetyl CoA and shuttles it into the citric acid cycle (TCA) for cellular respiration (Figure 3). The glycolytic pathway yields 2 molecules of ATP per molecule of glucose versus a whopping 38 ATP produced in aerobic metabolism. If lactate is not used or cleared it can cause pH to drop due to an increase in hydrogen ions, often leading to the familiar muscle fatigue associated with lactic acidosis.
Lactate is widely misunderstood and is often considered as a waste product from anaerobic metabolism. The truth is we make and use lactate all of the time (even when there is plenty of oxygen) and use it as a fuel and signaling molecule. Some muscle cells rely on it to function; fast-twitch muscle fibers convert glucose to lactate while slow-twitch muscle fibers are consumers of it. Lactate also is the preferred fuel source in the heart and brain and can be recycled back into glucose via the Cori cycle in the liver.
A recent study on ME/CFS patients showed elevated lactate in resting individuals, suggesting either increased anaerobic glycolysis or problems with the liver and/or muscle fibers. However, lactate may be adaptive in ME/CFS if this fuel substrate allows for patients to become more functional, bypassing some of the problems with oxidative energy production. This article here provides a general overview of the varied and important roles of lactate.
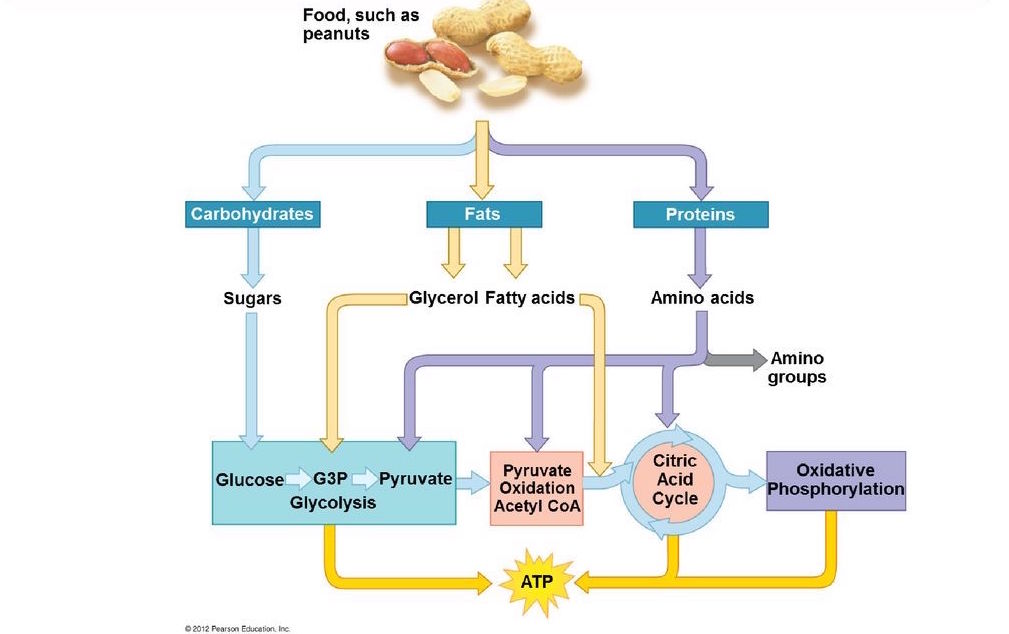
Aerobic system: The aerobic system is a three-part interconnected system, involving glycolysis, the citric acid cycle (also called the Krebs cycle or TCA), and oxidative phosphorylation. Glycolysis occurs in the cytoplasm (outside of mitochondria) whereas the TCA and oxidative phosphorylation occur in the mitochondria. Oxidative metabolism uses a broader number of substrates compared to anaerobic metabolism, including fatty acids and amino acids, in addition to glucose (see figure 6). In cancer cells, lactate can be produced in the presence of oxygen, a phenomenon known as the Warburg effect.
Several studies suggest aerobic metabolism is impaired at various points during cellular respiration. The PDH enzyme complex represents a pinch point in energy metabolism in ME/CFS and research also shows deficiencies in certain complexes in the electron transport chain used for oxidative phosphorylation. In addition, a growing number of studies also show impairments in the glycolytic pathway. In other words, our aerobic system is damaged in this disease.
An impaired aerobic system is reflected in decreased VO2 max (volume of oxygen consumed at maximum exercise intensity), a lower heart rate and VO2 at the anaerobic threshold (AT), and a lower workload at AT. The drop in function seen in repeat cardiopulmonary exercise testing (CPET) in ME/CFS also shows a damaged aerobic system.
Exercise intensity, fuels, and the anaerobic threshold
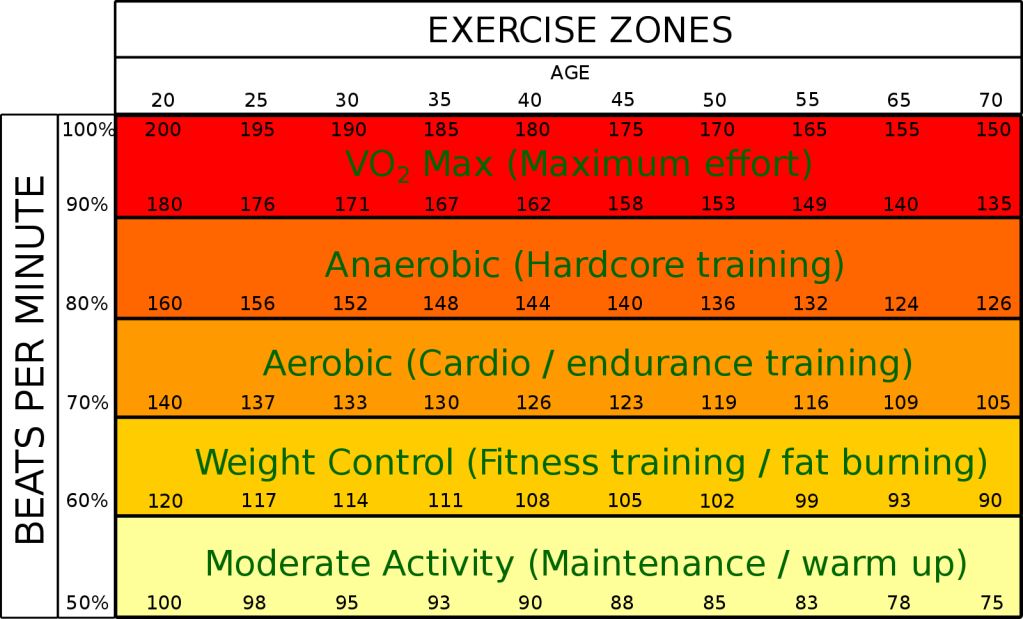
Another way to think about energy systems is in terms of fuels used as a function of exercise or activity intensity. Former athletes with ME/CFS may be familiar with exercise intensity zones, which are based on heart rate and age-predicted V02 max (see Figure 5). In the graph below (Figure 4) the anaerobic threshold occurs at the point at which sugar (CHO) becomes the predominant fuel. Beyond this point, energy is derived exclusively from the anaerobic system. In pacing, setting an alarm ~ 10% below AT can help people with ME/CFS avoid this zone.
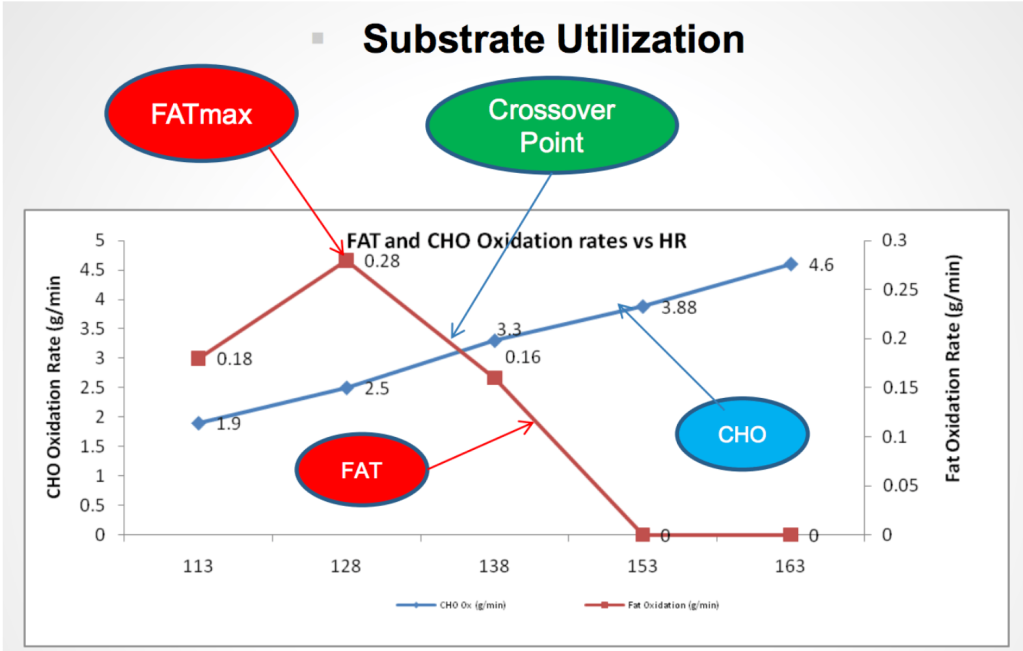
The two energy systems are not mutually exclusive until the anaerobic threshold has been surpassed. Even when we are below AT we use both aerobic and anaerobic energy systems.
What does a broken aerobic energy system mean in more practical terms for people with ME/CFS?
Many with ME/CFS experience PEM despite their best pacing efforts. Clearly, there is more to the story than simply staying under AT. My friend was urging us to focus on another aspect of pacing that often gets overlooked: avoiding aerobic activities by harnessing the anaerobic system.
She was interested in the portion of VanNess’s graph (Figure 1 above) showing that anaerobic glycolysis is the dominant energy system during the first two minutes of physical activity after being at rest. Even something as simple as sitting up in bed or standing briefly could trigger anaerobic metabolism. This system supplies rapid energy to muscles until more oxygen is on board. Following a brief period of anaerobic glycolysis, oxygen catches up to demand and we use a mix of glycolysis and fatty acid oxidation to fuel our bodies. Anaerobic metabolism can occur even while staying under AT.
VanNess also states in his talk that aerobic activities should be avoided. Say what? Hang on, aren’t we meant to avoid anaerobic metabolism by staying under our AT? Yes, this is true, but is not the whole story in pacing. However, this can lead people to think that as long as they stay under AT they are safe. Sadly, this is not true. The longer we are active in aerobic metabolism, the more likely PEM will occur.
If we are not meant to be in either aerobic or anaerobic metabolism for very long and the ATP-CP energy system is a very-short-lived, what is an ME patient to do?!?
This is where the nuance comes in. According to Staci Stevens at Workwell foundation, there isn’t a whole lot we can do about our broken aerobic system. It just is. This is why they are so outspoken against graded exercise therapy. In people with a functioning aerobic system, exercise can be done just under AT incrementally until there is more efficiency in that energy system. Not so in ME/CFS. Even with activities done under AT, symptom exacerbation can occur and more damage can be done to the aerobic energy system.
Staci Stevens tells a story about a Workwell client who set out to raise her VO2 and AT by gently walking a few days a week while under AT. When she returned to repeat her CPET she discovered she had experienced a significant drop in VO2 max and VO2 at AT, which is arguably the most important measure of function. This is what a damaged aerobic energy system does and why VanNess says to avoid using it.
Clearly, we spend most of our day in aerobic metabolism. Staci Stevens concedes of course it is rather absurd to think we can avoid aerobic metabolism. Instead, she encourages people to get curious and determine what level and duration of activity can be tolerated without going into PEM. For someone with severe illness, this could occur with only cognitive inputs, such as light and sounds. For others, such as myself (moderate-severe), it may be possible to sit up in bed and work on a computer for an hour or so. People on the mild end of the spectrum may be able to handle more activity. As any person with ME/CFS will tell you, it is not just physical activity that causes PEM.
The anaerobic paradox in pacing
On one hand, people embarking on a pacing program are advised to stay below AT to avoid being in anaerobic metabolism, yet on the other hand, we are told to do as much of our activities anaerobically. While this sounds like double-speak, VanNess explains why it is not in his video. There is a difference between allowing heart rate to climb until it has exceeded AT and continuing to do activity above AT (see figure 4) vs. harnessing the few minutes of anaerobic metabolism that we experience when we first start a physical activity after we have been at rest rest (see Figure 1). By avoiding the former and using the latter we can mitigate the worst impacts of being above AT and doing too much in aerobic metabolism.
Advanced pacing
Advanced pacers can build on this concept by training both the ATP-CP and anaerobic systems to be more efficient. Wait, now you are now telling me to go exercise? Yes, but not in the way that GET prescribes, which includes gradual and incremental training of the aerobic system. Instead, we are encouraged to do short-duration interval training so that we can train our anaerobic systems to be more efficient.
Training the anaerobic system increases intramuscular levels of ATP, CP, and glycogen, the quantity and activity of glycolytic enzymes, and tolerance to muscle fatigue. This gives us more energy to get our business done in short bursts, such as sitting up, going to the toilet, grabbing a snack, etc.
In general, training the ATP-CP energy system focuses on short bursts of activity for 5-10 seconds targeting muscles needed to perform desired activities. Training the glycolytic system focuses on short bursts of activity, for 30 seconds or less, including gravity-eliminated work, paired with energy conservation techniques (i.e., body positioning), strategic rest, and heart rate monitoring. This should only be attempted once far away from rolling PEM associated with the push/crash cycle and under the guidance of a physical therapist trained in Workwell’s methods. Given the variation in disease severity in ME/CFS, there is no one-size guidance that fits all. What counts as a suitable exercise for one person may be unsafe for another person.
This pacing method also requires a patient to tune in and recognize their immediate symptoms of PEM to avoid further symptom exacerbation. Workwell has an excellent graphic that breaks down the PEM time course, showing immediate, short-term, and long-term symptoms of PEM.
To read more about Workwell’s conceptual model for pacing see this 2010 paper. For pacing management, the paper suggests doing “therapeutic activities that last less than 2 minutes and are conducted at an intensity consistent with an HR that is 10% below the HR at the AT or rate of perceived exertion (RPE) below 13 to 15.”
Can the broken energy system be fixed?
No, and yes. As seen over and over, we cannot use aerobic training to increase the capacity of this energy system, as GET proponents would like us to believe. Recall the Workwell client who set out to “get in better shape” using her aerobic system.
Now to the “yes” part, the golden ticket in ME/CFS. A very small percentage of patients spontaneously recover – in most cases we will never know why. In others, such as the high profile cases of Jeffrey Wood and Jen Brea, a surgery addressing a mechanical problem (CCI) seemed to fix energy metabolism. Thirdly, the drug Ampligen helped to increase exercise tolerance. Hopefully, we’ll see new treatments that will help address this core component of the illness.
Until then, a smart pacing plan can help to improve function and minimize PEM.
Acknowledgements
I give my heartfelt thanks to Staci Stevens, M.A. and Todd Davenport, Ph.D. for taking time out of their busy lives to review this blog for accuracy.

This article fills a gap between the science and how to share it with medical providers–as well as with the exercise-literate family and friends who haven’t been able to get it about what happens for us. I am so grateful to have you in our community, though of course I’m sorry that you landed here.
LikeLike
Thank you for reading! I will be working with Staci and Todd to come up with a less “bloggy” version that can be shared. I’ll be sure to post the link when we finish it! Thank you so much for being such a big supporter – we are also so very lucky to have you in our community 🙂
LikeLike
Thank you for this, and all the work that you put into it! I’ve been trying to learn more and more about ME/CFS (only diagnosed 7 months ago) and this explains a lot of the things I’ve been experiencing since trying to maintain (and hopefully even improve) function yet my symptoms have gotten progressively worse. By each and every of the 9 different doctors that I’ve seen, I’ve been advised to exercise, and just make sure that my heartrate doesn’t go over AT. Being highly motivated to do whatever will help, I’ve been just doing that.And, of course it’s intuitive … but not for ME/CFS. I am SO thankful for this information!! Thank you.
LikeLike
Thank you so much! I tried this kind of exercise for 2 weeks and it seems to be pem save (tried up to 1 min intervals). Additionally I sometimes hold my breath after exhalation while doing exercise. Some month ago this kind of hypoxia has led to a few days of fatigue, but I hope, if done carefully and long-term, it leads to various positive effects I read about CFS/hypoxia, especially building up new mitochondria.
Could the limited supply of oxygen (breath holding) cause a delay/supression in the participation of the aerobic system? Maybe we can use the anaerobic system a bit longer when holding breath…
LikeLike
Hello Niko! How interesting that you have tried this approach and have seen that it doesn’t seem to exacerbate PEM. I am forever in rolling PEM and have been advised to NOT try this until am out of PEM (if such a thing is possible!). I am not sure about your question about holding your breath, but did you see Cort’s blog on hypocapnea? https://www.healthrising.org/blog/2019/02/01/hypocapnic-cerebral-hypoperfusion-orthostatic-intolerance-chronic-fatigue-syndrome/
Thanks for reading!
LikeLike
I´ve been reading your articles for a while and they´ve been really helpful in my trying to understand ME on a deeper level. So thank you! In this article one thing really struck me, and I´ve been thinking about it for a while; the cori cycle. Now, I´ve been getting frustrated by high bloodsugar in spite of a strict keto, wanting to get into deeper ketosis for better healing. I remembered what you wrote about the cori cycle, and did some more research on it. And that is where I think it got really interesting.
So… a body with ME, prone to produce overloads of lactic acid in the muscles even from very little exercise, builds up lactate that needs to be taken care of. Enters the cori cycle; recycling the lactic acid in the liver, producing glucose! Glucose enters the bloodstream, and voilá; blood sugar spikes, disturbing ketosis. Now, beeing homebound with extremely little energy it´s really hard not to overexert the muscles, and the more overexertion, the more glucose in the blood, right?
So. What to do about it, or is there even anything to do but try harder not to overexert? Considering the lactate as a helper in broken energy system, but a hindrance to medicinal ketosis. And that the fundamental problem still is lack of energy. What would you think about it?
LikeLike
Hello, Jenny! Thanks for reading my (rather impenetrable) blog! So many great observations and questions above – I agree, we need a better understanding of how our bodies use lactic acid, especially how much of it is being used a fuel—interesting thoughts on whether the Cori cycle could be throwing you out of ketosis.
I was struck by Neil McGregor’s talk at the 2019 Emerge conference discussing impaired glucose metabolism in ME/CFS patients, including a profile that looks like incipient metabolic syndrome. I am wondering if you fit one of the patterns he discusses? I know there is so much emphasis on impairments in oxidative energy production, but many researchers have found problems in the glycolytic pathway. I wish I better understood how to join up all of these ideas.
https://mecfsconference.org.au/videos/neil-mcgregor/
As an aside, I have been a big fan of Marty Kendell’s work. He developed a data-driven fasting approach using blood glucose levels to guide feeding. Combined with a low-carb/keto diet, I have seen remarkable success stories of people who had high fasting BG but brought it down simply by limiting eating to when BG reaches a certain level (determined by individual patterns). Do you also combine keto with time-restricted feeding?
I have good fasting BG levels and am underweight, so I have to be careful with fasting and time-restricted feeding, but it seems like a good approach to combine fasting with keto to better manage BG.
Thanks for reading my blog – I so appreciate your thought-provoking comment!
LikeLike
Please point me to papers that expand on this notion. “In general, training the ATP-CP energy system focuses on short bursts of activity for 5-10 seconds targeting muscles needed to perform desired activities.” I can’t find any research on this approach, though it makes perfect sense to focus on the energy system that isn’t broken!!
LikeLike
There are no papers looking at this specifically concerning ME/CFS, but several groups are starting to promote this idea, including Dr. Klimas and PTs working with Dr. Systrom. This talk by Mark VanNess is good.
Part 1: https://www.youtube.com/embed/FXN6f53ba6k
Part 2: https://www.youtube.com/watch?v=7BceGgEdMpA&feature=youtu.be
Workwell Foundation is working on new materials around pacing, including this more advanced topic. Stay tuned!
LikeLike
I’ve been doing 10 second intense bursts every day for 3 weeks. Weight lifting and sprinting. I’ve been progressing quickly in terms of increased resistance and speed. But my slow dog walk tolerance remains the same.
LikeLike
Excellent! Given what we have learned about aerobic metabolism, I am not surprised to hear that dog walking is still a struggle but that you can do some lifting! You inspire me! I am back to some strict pacing hoping that I can get out of the rolling PEM and consider doing something like we are trying. Have you ever thought about supplementing with a little creatine? I put it in my electrolyte mix, but given that it’s what powers the creatine-phosphate energy system – the one you use in the first moments of living and sprinting – seems to make a little sense? Just thinking out loud. I hope you can continue to build on this (but beware of that aerobic system – Workwell did a webinar on pacing with a heart rate monitor recently, and they shared a few stories about people who were afraid of reconditioning and tried increasing aerobic exercise (walking the dog) – only to discover that their CPET values worsened. Workwell will be doing a webinar later this year on the type of program you are trying – I will be sure to report back!
LikeLike
Hi Caroline, just wanted to give you an update. I continue to stress ATP-PC training (and yes, I’ve been taking creatine for years), and minimize aerobic activity. Weight lifting training results in normal conditioning improvements. Started at a 45lb deadlift…up to 100lb. Never any repercussions CFS wise. I do 10-15 second walking sprints several times a day. No repercussions. If I walk my dog for more than 15 minutes, slowly, I risk being wiped out for a few days. What an amazing dichotomy our CFS bodies are! Anyway…this article of yours has been a game changer. It feels good to deadlift and to be strong…even if I need to sit down or lie down a lot at a park! Thanks again. Paul.
LikeLike